Learninsta presents the core concepts of Biology with high-quality research papers and topical review articles.
Human Endocrine System Various Types and its Function
There are two glandular systems such as the exocrine glands and the endocrine glands. The exocrine glands secrete enzymes, saliva and sweat and have ducts that carry their substances to the membrane surfaces. Example: salivary gland and gastric gland. The endocrine glands, called ductless glands produce hormones and lack ducts; they release their hormone to the surrounding tissue fluid.
The hormones circulate around the body and eventually reach the target organs. Endocrine glands (Figure: 11. 1) include the pituitary, thyroid, parathyroid, pineal, adrenal, thymus and are also known as exclusive endocrine glands.
The hypothalamus along with its neural function also produces hormones and is considered as a neuro endocrine gland. In addition several organs such as pancreas, gastro intestinal tract epithelium, kidney, heart, gonads and placenta are also have endocrine tissues and are known as partial endocrine glands.
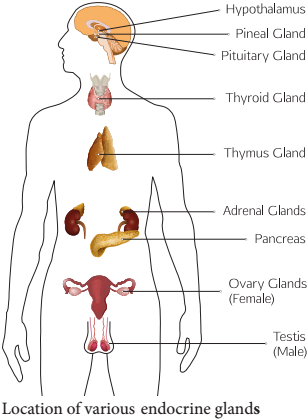
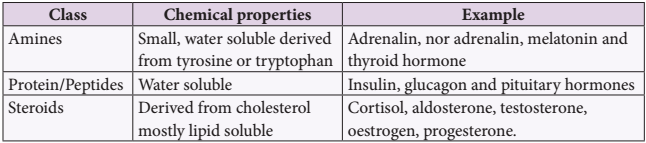
Table 11.1 Chemical Nature of Hormones
Hypothalamus
Hypothalamus is a small cone shaped structure that projects downward from the brain ending into the pituitary stalk. It interlinks both the nervous system and endocrine system. Though pituitary gland is known as master endocrine glands that controls the other endocrine glands, but it is, in turn controlled by the hypothalamus. Hypothalamus contains groups of neurosecretory cells. It produces neurotransmitters which regulate the secretions of the pituitary (Figure 11. 2). The hormones produced by the hypothalamus act either as a releasing hormone or as an inhibitory hormone.
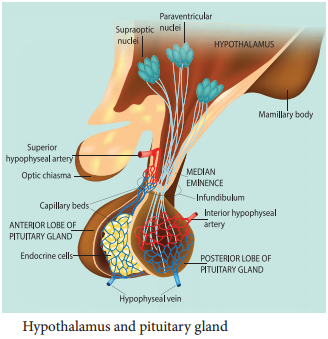
Table 11.2 The major hypothalamic hormones and their functions
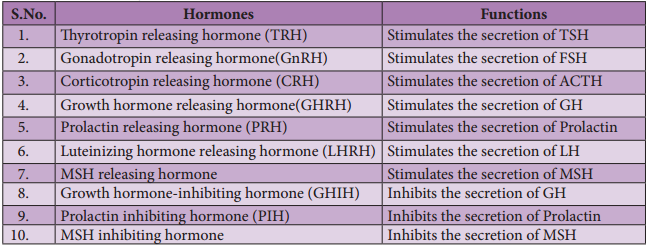
In the basal region of the brain, the hypothalamic hypophyseal portal blood vessel connects hypothalamus and anterior pituitary. It allows hypothalamic hormones to control anterior pituitary secretion. The posterior pituitary is connected with hypothalamus by a nerve bundle called hypothalamic hypophyseal axis. It produces nerve signal that control the posterior pituitary secretion. Hypothalamus maintains homeostasis, blood pressure, body temperature, cardio and fluid electrolyte balance of the body. As the part of limbic system it influences various emotional responses.
Pituitary Gland or Hypophysis
The pituitary gland (means to grow under) is ovoid in shape and is located in the sella turcica, a bony cavity of the sphenoid bone at the base of brain and connected to the hypothalamic region of the brain by a stalk called infundibulum. It is about one centimetre in diameter and 0.5 gm in weight. The pituitary consists of two lobes, anterior glandular adenohypophysis and posterior neural neurohypophysis.
The anterior lobe originates from the embryonic invagination of pharyngeal epithelium called Rathke’s pouch and the posterior lobe is originates from the base of the brain as an outgrowth of hypothalamus. Anatomically the adenohypophysis has three lobes or zones namely pars intermedia, pars distalis and pars tuberalis. The neurohypophysis is otherwise known as pars nervosa.
The anterior lobe of pituitary secretes six tropic hormones such as growth hormone (GH), thyroid stimulating hormone (TSH), adreno corticotropic hormone (ACTH), follicle stimulating hormone (FSH), luteinizing hormone (LH), luteotropic hormone (LTH) and melanocyte stimulating hormone (MSH) (in lower animals only). The posterior lobe of pituitary secretes the hormones namely vasopressin and oxytocin.
Hormones of Adenohypophysis
(i) Growth Hormone (GH):
It is also known as somatotropic hormone (STH) or Somatotropin. It is a peptide hormone. Growth hormone promotes growth of all the tissues and metabolic process of the body. It influences the metabolism of carbohydrates, proteins and lipids and increases the rate of protein biosynthesis in the cells.
It stimulates chondrogenesis (cartilage formation), osteogenesis (bone formation) and helps in the retention of minerals like nitrogen, potassium, phosphorus, sodium etc., in the body. GH increases the release of fatty acid from adipose tissue and decreases the rate of glucose utilization for energy by the cells. Thus it conserves glucose for glucose dependent tissues, such as the brain.
(ii) Throid Stimulating Hormone (TSH) or Thyrotropin:
TSH is a glycoprotein hormone, which stimulates the thyroid gland to secrete Tri-iodothyronine (T3) and thyroxine (T4). TSH secretion is regulated by negative feedback mechanism. It’s release from the anterior pituitary is induced by the thyrotropin releasing hormone (TRH). When thyroxine level in the blood increases, TRH acts on both the pituitary and hypothalamus to inhibit TSH secretion.
(iii) Adreno Cortico Tropic Hormone
(ACTH):
ACTH is a peptide hormone that stimulates the adrenal cortex to secrete glucocorticoids and mineralocorticoids. It stimulates melanin synthesis in melanocytes, induces the release of fatty acids from adipose tissues and stimulates insulin secretion. ACTH secretion is regulated by negative feedback mechanism.
(iv) Follicle Stimulating Hormone (FSH):
FSH is a glycoprotein hormone which regulates the functions of the gonads (ovary and testis). In males, FSH along with androgens acts on the germinal epithelium of seminiferous tubules and stimulates the production and release of sperms (spermatogenesis). In females, FSH acts on the ovaries and brings about the development and maturation of graffian follicles.
(v) Luteinizing Hormone (LH):
LH is a glycoprotein hormone which is also known as interstitial cell stimulating hormone (ICSH). In males, ICSH acts on the interstitial cells of testis to produce the male sex hormone, testosterone. In females, LH along with FSH matures the ovarian follicles.
LH independently induces ovulation, maintains the corpus luteum and promotes synthesis and release of ovarian hormones. FSH and LH are collectively referred as gonadotropins. FSH and LH are not produced during childhood. The secretion of FSH and LH starts only during pre pubertal period.
(vi) Luteotropic Hormone (LTH):
LTH is also called luteotropin or lactogenic hormone or prolactin or mammotropin. It is a protein hormone which stimulates milk secretion after the child birth in females. High prolactin secretion during lactation suppresses LH secretion and ovulation since it induces the corpus luteum hence named as luteo tropic hormone.
Hormones of Neurohypophysis
(i) Vasopressin or Antidiuretic Hormone (ADH) :
ADH is a peptide hormone which promotes reabsorption of water and electrolytes by distal tubules of nephron and thereby reduces loss of water through urine. Hence it is called as anti diuretic hormone. It also causes constriction of blood vessels when released in large amount and increases blood pressure. ADH deficiency causes Diabetes insipidus which induces the production of large amount of urine.
(ii) Oxytocin (Means Quick Birth):
It is a peptide hormone which stimulates vigorous contraction of the smooth muscles of uterus during child birth and ejection of milk from the mammary glands.
Pineal Gland
In human, the pineal gland or epiphysis cerebri or conarium is located behind the third ventricle of brain and is formed of parenchymal cells and interstitial cells. It secretes the hormone, melatonin, which plays a central role in the regulation of circadian rhythm of our body and maintains the normal sleep wake cycle. It also regulates the timing of sexual maturation of gonads. In addition melatonin also influences metabolism, pigmentation, menstrual cycle and defence mechanism of our body.
Thyroid Gland
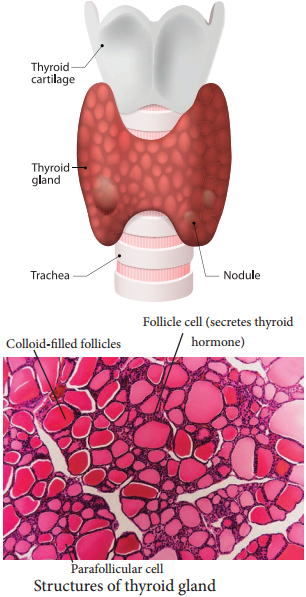
The butterfly shaped thyroid gland is a bilobed gland located below the larynx on each side of upper trachea. It is the largest endocrine gland in the body. Its two lateral lobes are connected by a median tissue mass called isthmus.
Each lobe is made up of many lobules. The lobules consist of follicles called acini (acinus in singular). Each acinus is lined with glandular, cuboidal or squamous epithelial cells. The lumen of acinus is filled with colloid, a thick glycoprotein mixture consisting of thyroglobulin molecules.
Hormones of the thyroid gland are often called the major metabolic hormones. The follicular cells of thyroid gland secrete two hormones namely tri-iodothyronine (T3) and thyroxine or tetra – iodothyronine (T4). The parafollicular cells or ‘C’ cells of thyroid gland secrete a hormone called thyrocalcitonin. Iodine is essential for the normal synthesis of thyroid hormones.
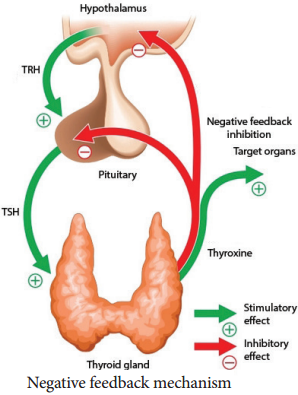
Thyroid releasing hormone from the hypothalamus stimulates the adenohypophysis to secrete TSH, which inturn stimulates the thyroid gland to secrete the thyroid hormones. Thyroid hormones show a negative feedback effect on the hypothalamus and pituitary (Figure 11. 3).
Functions of Thyroxine or Tetraiodothyronine (T4):
Thyroxine regulates the basal metabolic rate (BMR) and body heat production. It stimulates protein synthesis and promotes growth. It is essential for the development of skeletal and nervous system. Thyroxine plays an important role in maintaining blood pressure. It reduces serum cholesterol levels, Optimum levels of thyroxine in blood is necessary for gonadial functions.
TCT is a polypeptide hormone, which regulates the blood calcium and phosphate levels. It reduces the blood calcium level and opposes the effects of parathyroid hormone.
Parathyroid Gland
In human, four tiny parathyroid glands are found in the posterior wall of the thyroid glands. This gland is composed of two types of cells, the chief cells and oxyphil cells. The chief cells secrete parathyroid hormone (PTH) and the functions of oxyphil cells are not known.
Parathyroid Hormone or Parathormone (PTH)
PTH is a hypercalcemic hormone. It is a peptide hormone involved in controlling the calcium and phosphate homeostasis. The secretion of PTH is controlled by calcium level in the blood. It increases the blood calcium level by stimulating osteoclasts to dissolve the bone matrix.
As a result calcium and phosphate are released into the blood. PTH enhances the reabsorption of calcium and excretion of phosphates by the renal tubules and promotes activation of vitamin D to increase calcium absorption by intestinal mucosal cells.
Thymus Gland
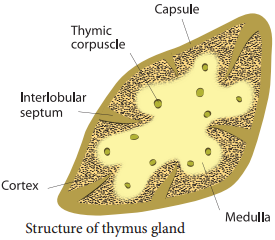
Thymus gland is partially an endocrine and partially a lymphoid organ. It is a bilobed structure located just above the heart and aorta, behind the sternum. It is covered by firous capsule and anatomically it is divisible into an outer cortex and an inner medulla.
It secretes four hormones such as thymulin, thymosin, thymopoietin and thymic humoral factor (THF). The primary function of thymus is the production of immuno competent ‘T’ lymphocytes which provides cell mediated immunity.
Adrenal Gland
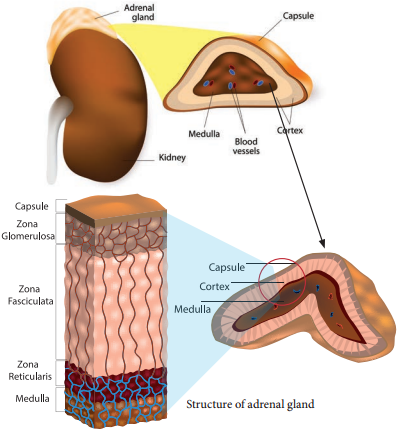
A pair of adrenal glands are located at the anterior end of the kidneys, hence also called suprarenal glands. Anatomically the outer region is the cortex and the inner region is the medulla. Histologically the adrenal cortex has three distinct zones, zona glomerulosa, zona fasciculata and zona reticularis.
Zona glomerulosa an outer thin layer constitutes about 15% of adrenal cortex, and secretes mineralocorticoids. Zona fasciculata, the middle widest layer constitutes about 75% of adrenal cortex and secretes glucocorticoids such as cortisol, corticosterone and trace amounts of adrenal androgen and oestrogen. Zona reticularis, an inner zone of adrenal cortex constitute about 10% of adrenal cortex and secretes the adrenal androgen, trace amount of oestrogen and glucocorticoids.
Adrenal Medulla:
It is the central part of adrenal gland and is composed of ovoid and columnar cells, which are found around the network of blood capillaries. Adrenalin (epinephrine) and nor adrenalin (nor epinephrine) are the two hormones secreted by the adrenal medulla. Both adrenalin and nor adrenalin are catecholamines.
Function of Adrenal Hormones:
Glucocorticoids stimulate gluconeogensis, lipolysis and proteolysis (the life saving activity). Cortisol is a glucocorticoid involved in maintaining cardio vascular and kidney functions. It produces anti inflammatory reactions and suppresses the immune response.
It stimulates the RBC production. It is also known as stress combat hormone. Mineralocorticoids regulates water and electrolyte balance of our body. Aldosterone stimulates the reabsorption of sodium and water and eliminates potassium and phosphate ions through excretion, thus it helps in maintaining electrolytes, osmotic pressure and blood pressure. Adrenal androgen plays a role in hair growth in the axial region, pubis and face during puberty.
The adrenal medulla secretes the hormones adrenalin and noradrenalin and are referred as “3F hormone” (fight, flight and fright hormone). Adrenalin increases liver glycogen breakdown into glucose and increases the release of fatty acids from fat cells.
During emergency it increases heart beat rate and blood pressure. It stimulates the smooth muscles of cutaneous and visceral arteries to decrease blood flow. It increases blood flow to the skeletal muscles thereby increases the metabolic rate of skeletal muscles, cardiac muscles and nervous tissue.
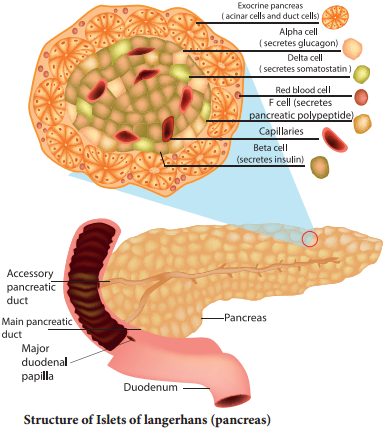
Pancreas
Pancreas is a composite gland which performs both exocrine and endocrine functions. It is located just below the stomach as a leaf like structure. The pancreas is composed of two major tissues such the acini and islets of langerhans.
Acini secretes digestive enzymes and the islets of langerhans secretes hormones like insulin and glucagon. Human pancreas has one to two million islets of langerhans. In each islet about 60% cells are beta cells, 30% cells are alpha cells and 10% cells are delta cells. The alpha cells secrete glucagon, the beta cells secrete insulin and delta cells secrete somatostatin.
Insulin:
Insulin is a peptide hormone and plays an important role in glucose homeostasis. It’s main effect is to lower blood glucose levels by increasing the uptake of glucose into the body cells, especially muscle and fat cells. Insulin also inhibits the breakdown of glycogen to glucose, the conversion of amino acids or fats to glucose, so insulin is rightly called a hypoglycemic hormone.
Glucagon:
Glucagon is a polypeptide hormone. It is a potent hyperglycemic hormone that acts on the liver and promotes the breakdown of glycogen to glucose (Glygogenolysis), synthesis of glucose from lactic acid and from non-carbohydrate molecules (Gluconeogenesis).
Glucagon releases glucose from the liver cells, increasing the blood glucose levels. Since glucagon reduces the cellular uptake and utilisation of glucose it is called a hyperglycemic hormone. Prolonged hyperglycemia leads to the disorder called diabetes mellitus.
Gonads
Testis:
A pair of testis is present in the scrotal sac of males. The testis functions as a sex organ and also as an endocrine gland. The testis is composed of seminiferous tubules and interstitial cells or Leydig cells. The Leydig cells secrete several male sex hormones, collectively called androgens, mainly testosterone.
Functions of Testosterone:
Under the influence of FSH and LH, testosterone initiates maturation of male reproductive organs, and the appearance of secondary sexual characters, muscular growth, growth of facial and axillary hair, masculine voice and male sexual behaviour. It enhances the total bone matrix and plays a stimulating role in the process of spermatogenesis.
Ovary:
Females have a pair of ovaries located in the pelvic region of the abdomen. The ovary is composed of ovarian follicles and stromal tissues. It produces the eggs or ova. The ovaries secrete the steroid hormones oestrogen and progesterone. Oestrogen is responsible for the maturation of reproductive organs and the development of secondary sexual characters at puberty.
Along with progesterone, oestrogens promotes breast development and initiate the cyclic changes during menstrual cycle. Progesterone prepares the uterus for implantation of the fertilized ovum. It decreases the uterine contraction during pregnancy and stimulates the development of mammary glands and milk secretion. It is responsible for premenstrual changes in the uterus and is essential for the formation of placenta.
Hormones of Heart, Kidney and Gastro Intestinal Tract
Some tissues of the heart, kidney and gastro intestinal tract acts as partial endocrine glands. In the heart, cardiocytes on the atrial wall’s secretes an important peptide hormone called atrial natriuretic factor (ANF). When blood pressure is increased, ANF is secreted and causes dilation of the blood vessels to reduce the blood pressure.
In kidneys, hormones such as renin, erythropoietin and calcitriol are secreted. Renin is secreted by juxta glomerular cells (JGA), which increases blood pressure when angiotensin is formed in blood. Erythropoietin is also secreted by the JGA cells of the kidney and stimulates erythropoiesis (formation of RBC) in bone marrow. Calcitriol is sercreted by proximal tubules of nephron. It is an active form of vitamin D3 which promotes calcium and phosphorus absorption from intestine and accelerates bone formation.
Gastro Intestinal Tract Hormones
Group of specialized endocrine cells present in gastro-intestinal tract secretes hormones such as gastrin, cholecystokinin (CCK), secretin and gastric inhibitory peptides (GIP). Gastrin acts on the gastric glands and stimulates the secretion of HCl and pepsinogen.
Cholecystokinin (CCK) is secreted by duodenum in response to the presence of fat and acid in the diet. It acts on the gall bladder to release bile into duodenum and stimulates the secretion of pancreatic enzymes and its discharge. Secretin acts on acini cells of pancreas to secrete bicarbonate ions and water to neutralize the acidity. Gastric inhibitory peptide (GIP) inhibits gastric secretion and motility.